What is coeliac disease?
Coeliac disease has a wide range of symptoms that affects different people in different ways, so diagnosis can sometimes be tricky.
It currently takes, on average, 13 years from when someone first experiences symptoms to diagnosis, and a quarter of those with coeliac disease were previously misdiagnosed with Irritable Bowel Syndrome (IBS).
Coeliac disease (pronounced see-liac) is a lifelong autoimmune condition where the body’s immune system reacts to gluten, a protein found in wheat, barley and rye. The body’s reaction to gluten causes damage to the lining of the intestine, the place where food and nutrients are absorbed. This deprives the body of the nutrients it needs and can lead to malnutrition.
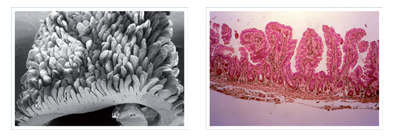
Healthy Intestine
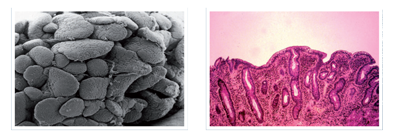
Intestine damaged by coeliac disease, G.B. Gasbrinni and F. Mangiola, 2014
What are the symptoms?
People often report typical gut symptoms, but other parts of the body can also be affected. The most commonly reported symptoms are:
-
frequent bouts of diarrhoea or loose stools
-
nausea, feeling sick and vomiting
-
stomach pain and cramping
-
lots of gas and bloating
-
feeling tired all the time, ongoing fatigue
-
anaemia (you would be told if you’re anaemic following a blood test)
-
weight loss (although not in all cases)
-
regular mouth ulcers
-
constipation or hard stools
-
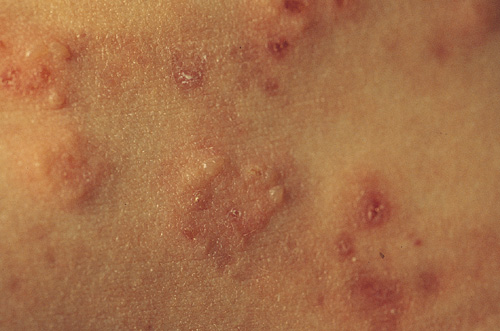
skin rash (dermatitis herpetiformis, the skin manifestation of coeliac disease, see image below)
Who is at risk?
Around one in 100 people has coeliac disease. If you have a first degree family member (parent, sibling or child) with the condition, then your chances of having the condition increase to one in 10.
People with coeliac disease are also more likely to have other autoimmune conditions, including Type 1 diabetes and autoimmune thyroid disease. If you have one of these conditions, it is important that you are also tested for coeliac disease.
Many people with coeliac disease have previously been diagnosed with Irritable Bowel Syndrome (IBS), as the symptoms often look similar. If you have been diagnosed with IBS in the past, still have symptoms, and haven’t been checked for coeliac disease before, you should ask to be tested.
How do I go about getting diagnosed?
The first step to getting diagnosed with coeliac disease is to have a simple blood test at your GP surgery. The test looks for the antibodies produced by people with coeliac disease when they eat foods containing gluten. It is essential to keep eating gluten before and throughout the testing process, otherwise your body won’t produce antibodies, and you could get a false negative result. Gluten must be eaten in more than one meal every day for six weeks before testing.
If the blood test is positive you will be referred for an endoscopy with a biopsy. This involves a small camera being passed through your mouth and stomach, then into the small bowel. Small samples of the lining of the small bowel are collected and then looked at for signs of coeliac disease.
Although diagnosis of coeliac disease generally involves having a blood test and then an endoscopy with biopsy, for some children, a biopsy may not be needed.
What types of foods contain gluten?
Gluten is a protein found in wheat, barley and rye. The types of foods that typically contain gluten are bread, cereal, pasta, cakes, pastries and biscuits. It can also be found in less obvious places such as sausages, stock cubes and soy sauce.
What do I do if I’ve already removed gluten from my diet?
If you have removed gluten from your diet for any reason, it is pointless being tested for coeliac disease. This is because the blood test looks for the antibodies produced by people with coeliac disease when they eat gluten. If you have stopped eating gluten, your body will not be producing the antibodies that are identified by the blood test.
The only way around this is to start eating gluten again. This is normally referred to as the ‘gluten challenge’. You will need to include gluten in your diet for six weeks before having a blood test. Gluten should be included in more than one meal every day, or around the equivalent of four slices of bread per day for six weeks.
For those with undiagnosed coeliac disease this could mean a return of symptoms. So it is important you discuss the gluten challenge with your GP before taking this step.
What is the treatment?
Here is the good news. There is a complete treatment for coeliac disease and it can be treated without medication. Currently, the only treatment for coeliac disease is a gluten-free diet. Once gluten has been removed from your diet, you will begin to heal and symptoms will usually improve in a few weeks. It can take between two and five years for the gut to fully heal.
For more information about the gluten-free diet and lifestyle please visit the Coeliac Society of Ireland website.
Why is being properly diagnosed important?
Getting your GP to confirm a diagnosis of coeliac disease is important. Firstly to ensure your symptoms are not another medical problem. The symptoms of coeliac disease can be similar to other medical conditions, so it is important to be properly tested by your GP.
Complications associated with coeliac disease include osteoporosis and in rare cases, small bowel cancer.
Coeliac disease is genetic, which means there is a higher chance of you having the condition if one of your immediate relatives has a diagnosis, but it is not passed within families in a predictable way. Diagnosis is important so that relatives who develop symptoms know to be tested.
What should I do next?
If you think you may have coeliac disease, you should book an appointment with your GP to discuss your concerns and get a blood test.
If you’re still a little unsure, you might find it useful to take our online assessment. This short questionnaire will take you through the symptoms of coeliac disease and other risk factors. Once complete, you will be sent the results with a recommendation about further testing.
If you would like further details about coeliac disease, there is more information on the Coeliac Society of Ireland website.
Can I speak to a person?
Yes. Coeliac Society of Ireland operates a Helpline which is available to all. Our Helpline is staffed Monday to Friday from 9am to 5pm. Please call 01-8721471.
You can also email the Helpline about diagnosis at info@coeliac.ie.
Our Helpline staff can also talk to you about any additional support you might require. Experienced Members are teamed up with people wanting some additional peer support. If you’re interested in this service, please talk to our Helpline staff who will be able to tell you more.
